
Prof Mason
Liverpool Foot and Ankle Clinic
To book an appointment, either email or phone the number below or click the link.
E-mail: CVDWclerical@outlook.com
Contact Patient Liaison: 07717580737

Mr Lampridis
Liverpool Foot and Ankle Clinic
To book an appointment, either email or phone the number below or click the link.
E-mail: Oaklands.PrivatePatient@ramsayhealth.co.uk
Contact Patient Liaison: 01617877700
Complex Regional Pain Syndrome (CRPS)

What is CRPS?
Complex regional pain syndrome, usually called CRPS, is a pain condition that most often affects an arm, hand, leg or foot. It usually starts after an injury, fracture, operation, sprain, or sometimes even a relatively minor event. The pain is typically more severe and lasts longer than would normally be expected for the original problem.
CRPS can also cause changes in skin colour, skin temperature, swelling, sweating, movement, hair, nails and sensation. Some people describe burning pain, extreme sensitivity to touch, stiffness, weakness, or a feeling that the limb does not feel normal.
Although CRPS can be very distressing,
early recognition and treatment are important, and many people improve with the right support and rehabilitation.
How common is CRPS?
CRPS is uncommon, but not rare.
- After most injuries or operations, the vast majority of patients do not develop CRPS
- Studies suggest it occurs in roughly 1–5% of patients after fractures
- After foot and ankle surgery, reported rates are generally low (often around 1–2%), although this varies depending on the type of surgery and patient factors
It is important to emphasise that CRPS is not something that routinely happens after surgery, but it is something clinicians remain aware of so it can be recognised early if it does occur.
Why does CRPS happen?
The exact cause is not fully understood. Current evidence suggests that CRPS involves an abnormal response of the nervous system after an injury.
This can include:
- increased sensitivity of pain nerves
- changes in how the brain processes pain
- abnormal control of blood flow and temperature
- ongoing inflammation
In simple terms, the body develops an
overactive pain response. Even when the tissues have healed, the pain system can remain switched on.
Who is more at risk of developing CRPS?
There is no single cause, but certain factors appear to increase the risk:
Injury-related factors
- fractures (especially wrist and ankle fractures)
- surgery, particularly after trauma
- severe soft tissue injury
- prolonged immobilisation (long periods in a cast or boot)
Patient-related factors
- previous history of CRPS (increases risk in another limb)
- nerve injury associated with the original problem
- high levels of pain early after injury
- smoking
- some evidence suggests higher rates in women and people aged 40–60
Psychological and social factors
- anxiety or low mood
- fear of movement or re-injury
- stressful life circumstances
It is important to stress that
these are risk factors, not causes, and many people with these factors
never develop CRPS, while others without any obvious risk factors may still develop it.
What are the symptoms?
Symptoms vary from person to person, but commonly include:
- burning, deep or persistent pain
- pain from light touch (for example, socks or bed sheets)
- swelling in the foot or ankle
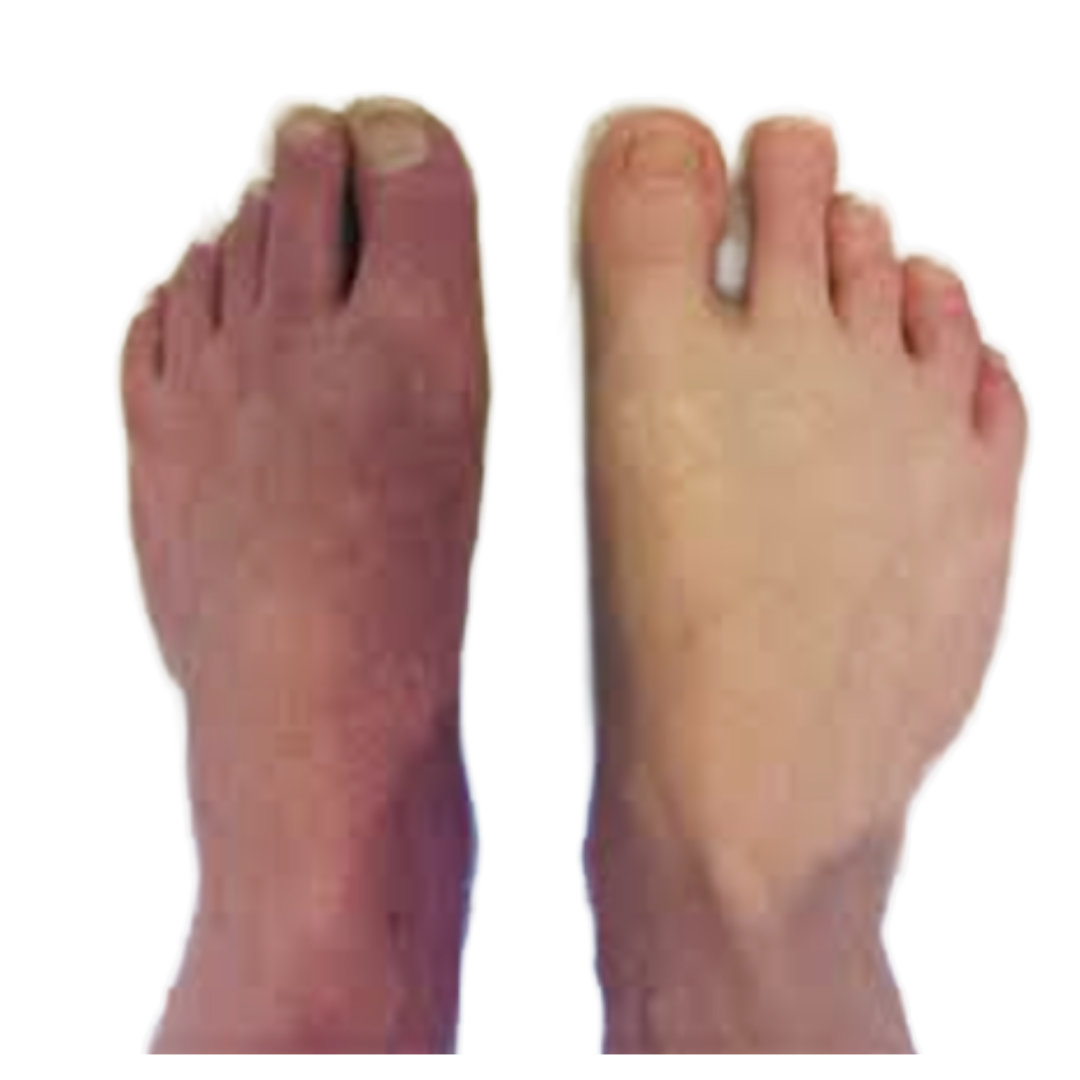
- changes in skin colour (red, purple, pale or blotchy)
- the foot feeling unusually hot or cold
- sweating changes
- stiffness or reduced movement
- weakness or poor control
- changes in hair, nails or skin
How is CRPS diagnosed?
There is no single test or scan that confirms CRPS. Diagnosis is based on symptoms, examination, and ruling out other causes such as infection, instability, arthritis or nerve compression.
Doctors commonly use the Budapest criteria.
Budapest criteria
To diagnose CRPS:
- There must be ongoing pain that is out of proportion to the original injury
- There must not be a better explanation for the symptoms
In addition, symptoms and signs must be present in different groups:
1. Sensory - Increased sensitivity or pain from light touch
2. Vasomotor - Temperature or colour differences
3. Sudomotor / swelling - Swelling or sweating changes
4. Motor / trophic - Stiffness, weakness, tremor, or changes in skin, hair or nails
Patients must report symptoms in
at least three groups, and the doctor must observe signs in
at least two groups.
CRPS Treatment
Treatment works best when started early and when multiple approaches are used together.
Education and reassurance
Understanding the condition is key. Knowing that the pain is real but comes from an overactive pain system can help reduce fear and improve recovery.
Pain relief
Medications may help control symptoms enough to allow movement and rehabilitation. These are tailored to the individual and are often specific to nerve pain.
Physiotherapy and rehabilitation
This is one of the most important treatments.
The aim is to:
- keep the foot and ankle moving
- gradually return to normal use
- reduce stiffness and sensitivity
- rebuild confidence
Psychological support
Chronic pain affects mood, sleep and confidence. Support such as pain management strategies or CBT can be very helpful as part of overall recovery.
Are specialist treatments ever needed?
If symptoms are severe or not improving, referral to a pain specialist may be appropriate.
In selected cases, treatments such as:
- nerve-targeted pain procedures
- spinal cord stimulation
- dorsal root ganglion stimulation may be considered.
What can you do to help?
- Try to keep the foot and ankle moving as much as you comfortably can
- Follow your physiotherapy programme closely, even if progress feels slow
- Avoid complete rest — not using the limb can make symptoms worse
- Build up activity gradually, rather than doing too much too soon
- If the area is very sensitive, gentle desensitisation techniques can help reduce pain over time
- Seek advice early if your symptoms feel more severe than expected or are not improving

